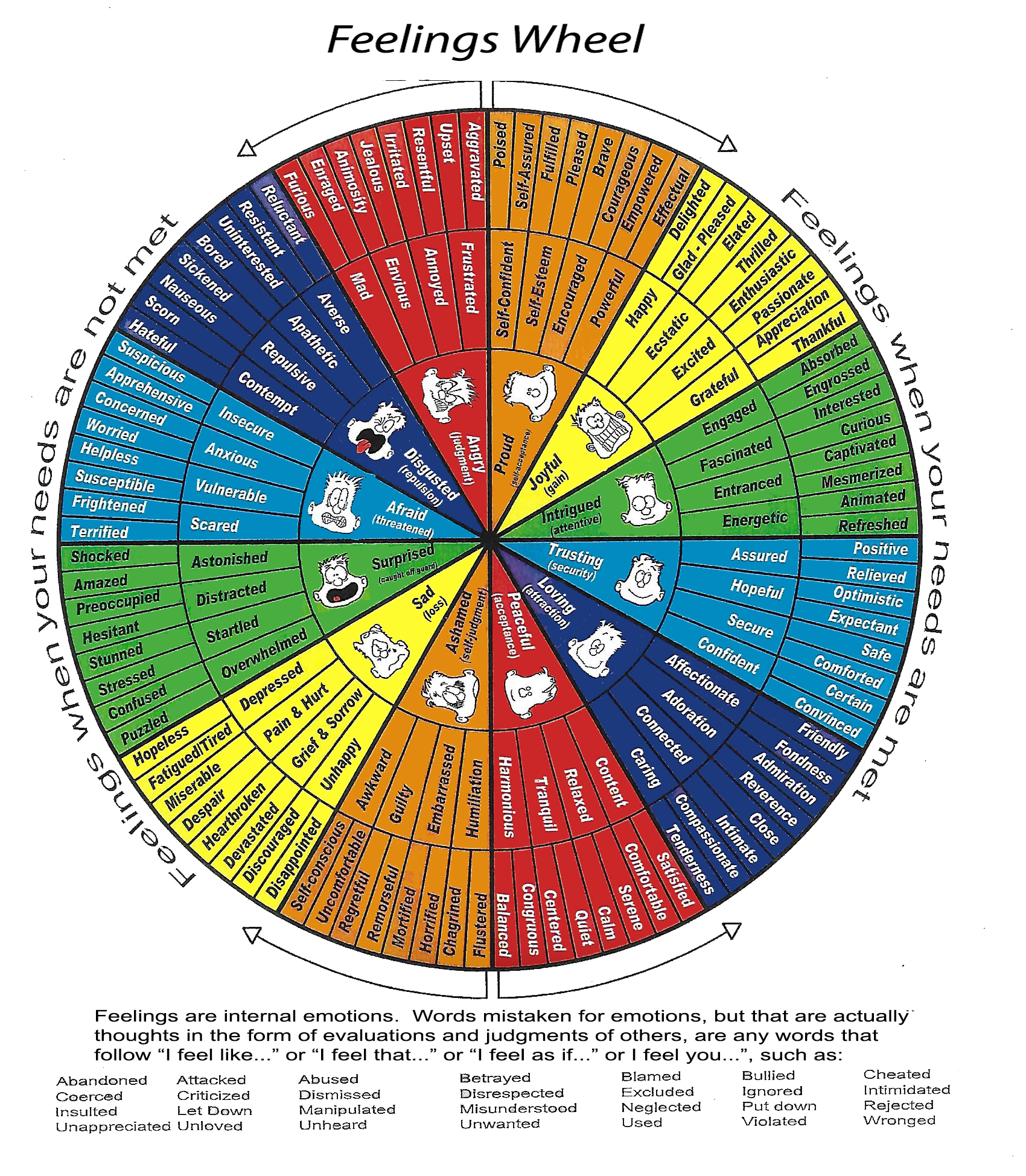
PTSD Therpy
There are many types of therapy the Mental Health Department uses to help you. Which one they choose depends on your condition. This page covers a few of them. Many are taught in PTSD Groups. You do not share your experiences in these groups. Talk with your therapist about which one would be beneficial for you. The instructor MUST BE IN TOTAL CONTROL of the group. Make sure a few of those attending are not in control. It will ruin the experience and you will not want to return if you have a weak instructor.
1. Some have to see things to understand what is being said.
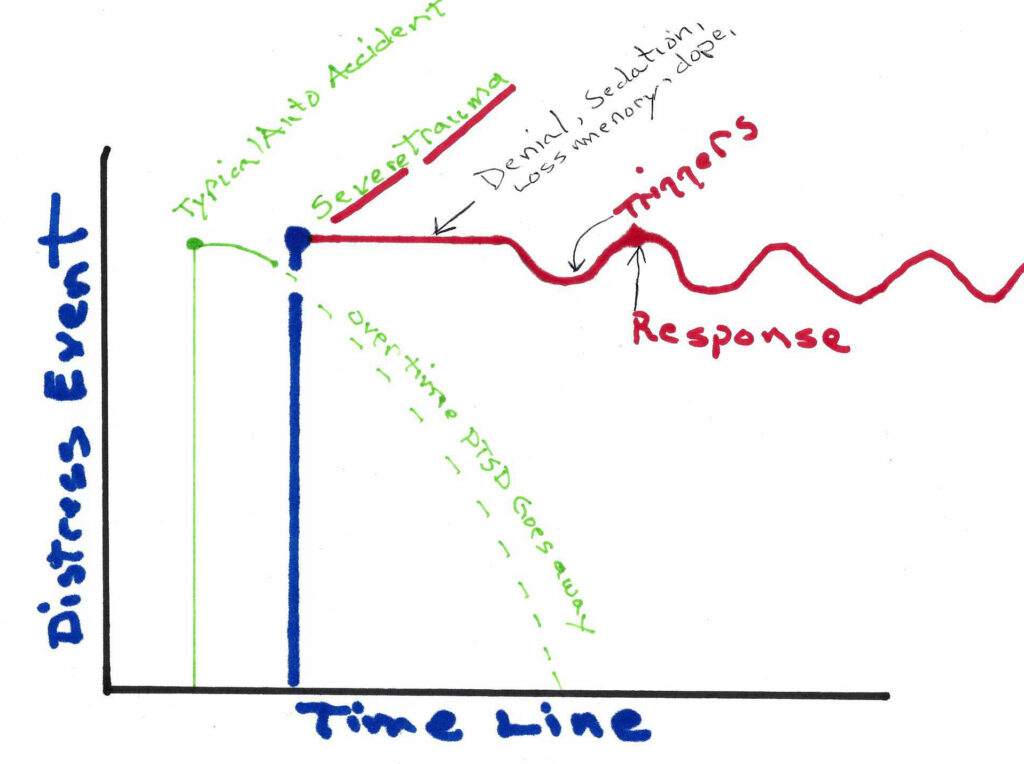
This chart gives clarity on why PTSD continues to this day. A typical trauma, like an accident, may cause PTSD but over time it goes away. It might flare up if the accident severely injured you. Severe Trauma does not go away so easily. When the event happens your mind may hide the event or substance abuse is used to feel normal. Something triggers you and you respond to it. It goes back down again then another trigger makes you experience the same trauma. Of course, during your time in combat, you will have many events that cause PTSD. This chart shows one event. There would be many events going up from the timeline causing more trauma you cannot cope with. You may be prescribed medication to flatten the stress you live with but something will trigger you to still have the same ups and downs responses caused by PTSD. At least this is how I interpreted that part of the class.
- Acute trauma results from a single incident.
- Chronic trauma is repeated and prolonged such as domestic violence or abuse.
- Complex trauma is exposure to varied and multiple traumatic events, often of an invasive, interpersonal nature
2. Big “T” and little “t” traumas By Chris Clancy:
“There are two main categories of trauma commonly referred to as Big “T” and little “t.” Big “T” traumas are the events most commonly associated with post-traumatic stress disorder (PTSD) including serious injury, sexual violence, or life-threatening experiences. Threats of serious physical injury, death, or sexual violence can cause intense trauma even if the person is never physically harmed. Witnesses to big “T” events or people living and working in close proximity to trauma survivors are also vulnerable to PTSD, especially those who encounter emotional shocks like paramedics, therapists, and police officers.
Little “t” traumas are highly distressing events that affect individuals on a personal level but don’t fall into the big “T” category. Examples of little “t” trauma include non-life-threatening injuries, emotional abuse, death of a pet, bullying or harassment, and loss of significant relationships. People have unique capacities to handle stress, referred to as resilience, which impacts their ability to cope with trauma. What is highly distressing to one person may not cause the same emotional response in someone else, so the key to understanding little “t” trauma is to examine how it affects the person rather than focusing on the event itself.
3. The accumulation of Stress and/or feeling a state of a Threat can shrink our Window of Tolerance. Once pushed outside our Window of Tolerance, it can become very difficult to take in new information. This is because these states of Hyper-arousal and Hypo-arousal are ancient physiological survival mechanisms that are shared across species throughout the entire animal kingdom.

4.
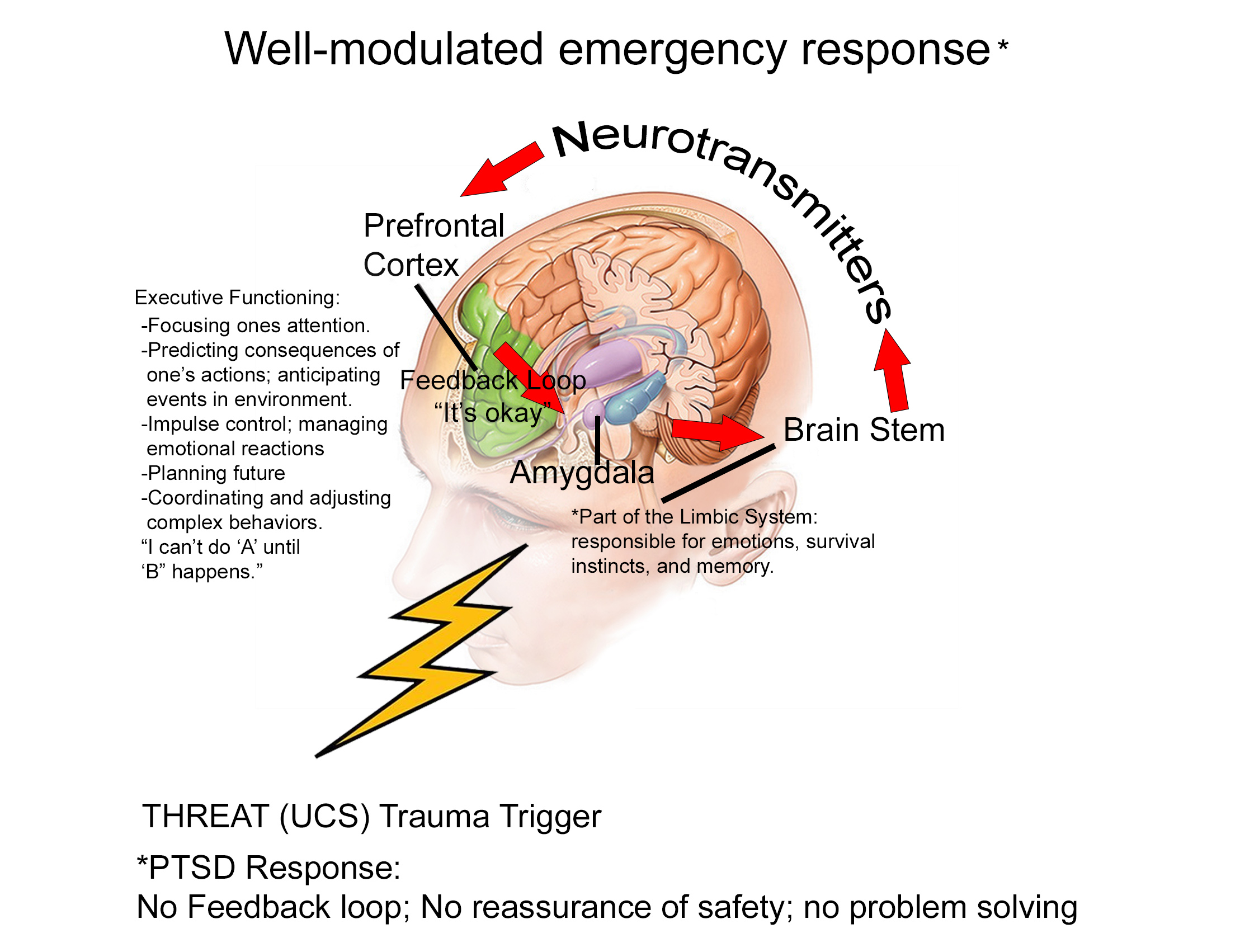
Our Neurotransmitters respond to threats allowing our Amygdala to make us relive the trauma caused by PTSD. You truly hear, see, feel, and taste what happens created by the neurotransmitter in our Amygdala. Talk to your VA Counselor about this. This is the teaching aid and is impossible to explain. Talk to a professional about this.
The amygdala is a structure in the brain’s limbic system (known as the emotional seat of the brain) that helps determine whether or not a threat is approaching, and if so, sends out a danger signal, initiates the fight-or-flight response, and then helps indicate when the threat is gone. When one has experienced trauma, the amygdala remains hyper-alert to even non-threatening stimuli and activates the fight-or-flight response system despite being safe. While experiencing PTSD, the brain can get caught up in a highly alert and activated loop during which it looks for and perceives threats everywhere. Mindfulness Practice
5. . Did you know CPT Cognitive Processing Therapy focused on rape victims originally? This therapy has also been successful with a range of other traumatic events, including military-related traumas and PTSD. Read and try to understand this. This Cognitive Processing Therapy Veteran/Military Version: THERAPIST’S MANUAL
6. Neuroplasticity The Science of Trauma, Mindfulness, and PTSD is also known as brain plasticity, neuroplasticity, or neural plasticity, which is the ability of the brain to change continuously throughout an individual’s life. That leads to Mindfulness-Based Cognitive Therapy or Meditation. You learn how to use cognitive methods and mindfulness meditation to interrupt the automatic processes often triggering depression. Trauma and PTSD changed our BRAINS. It is a VERY Deep Subject. Maybe this can help others. The VA uses medication for Neurological Treatments. However, they do talk about neuroplasticity in this PDF The nervous system is dynamic and plastic. It is not hard-wired! This adaptability is known as neuroplasticity, or the brain’s ability to reorganize itself by forming new neural connections throughout life. My next step is to find out more about this treatment called Targeted Neuroplasticity Training (TNT) by Dr. Tristan McClure-Begley This is something I will not try to do on my own.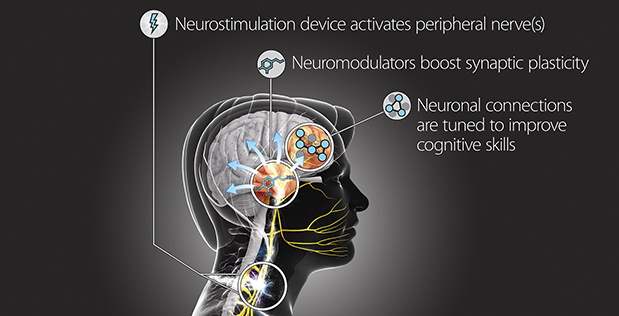
Mindfulness: A state of nonjudgmental awareness of what’s happening in the present moment, including the awareness of one’s own thoughts, feelings, and senses. That is hard for me to wrap my mind around.
Components of Mindfulness Awareness. During a state of mindfulness, you will notice your thoughts, feelings, and physical sensations as they happen. The goal isn’t to clear your mind or to stop thinking—it’s to become aware of your thoughts and feelings, rather than getting lost in them. Acceptance. The thoughts, feelings, and sensations that you notice should be observed in a nonjudgmental way. such as, if you notice a feeling of nervousness, simply state to yourself: “I notice that I am feeling nervous”. There’s no need to further judge or change the feeling.
Benefits of Mindfulness
- Reduced symptoms of depression and anxiety
- Improved memory, focus, and mental processing speed
- Improved ability to adapt to stressful situations
- Greater satisfaction within relationships
- Reduced rumination (repetitively going over a thought or problem)
- Improved ability to manage emotions

8. Behavioral Activation for Depression. There is so much information about this topic. Here is the lesson plan PDF. These are the first two paragraphs of this lesson plan.
 Have you ever noticed that certain things that you do influence your mood or anxiety? Such as: When you listen to sad music do you ever notice feeling sad for long periods of time? Do you ever feel less motivated to apply for a job or school when you are actively worrying?
Have you ever noticed that certain things that you do influence your mood or anxiety? Such as: When you listen to sad music do you ever notice feeling sad for long periods of time? Do you ever feel less motivated to apply for a job or school when you are actively worrying?
Behavioral activation is one of the most important CBT skills used in treating depression. It has to do with the way that behaviors and feelings influence each other.
A big part of this lesson was about the exploration of Values, Pleasure, Mastery, and Goals. To feel more consistently engaged and happy in the world, it is usually best to find a balance of goals centered on values, pleasure, mastery, and value-driven behavior. There are huge lists of these items you can do to help with depression. Again Here is the lesson plan PDF.
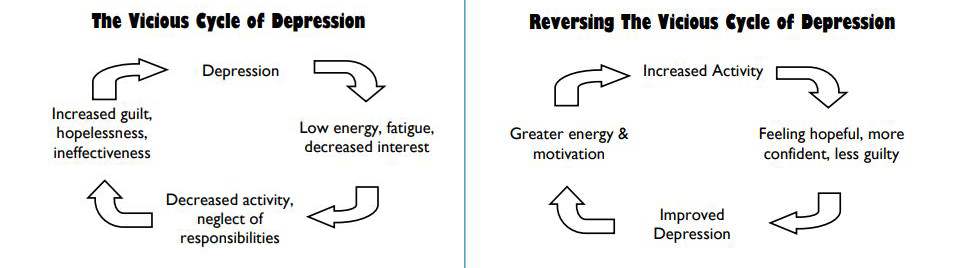
Another part of today’s class was about The Vicious Cycle of Depression. The symptoms of depression can bring about some drastic changes in a depressed person’s life, daily routines, and behavior. Often it is these changes that make the depression worse and prevent the depressed person from getting better. Here is that lesson plan. There is a vicious cycle of depression PDF.
LEARN HOW TO DO THIS…
Go to the YouTube Channel for The Center for Clinical Interventions (CCI). It is a specialist clinical psychology service in Perth, Western Australia, administered through the North Metropolitan Health Service. For more information about CCI, please visit https://www.CCI.health.wa.gov.au/
9. PTSD Anger Management. The Anger Iceberg and The Cycle of Anger.
10. How To Anchor Yourself With The 54321 Grounding Method
The 54321 grounding technique is simple, yet powerful. Like gradually attaching anchors to the boat, this method slowly pulls you back to earth.
First, take a moment to become mindful of your breath. Just a few deep breaths invite your body back into the moment, slowing everything down. Then, become aware of your environment.
- Look For 5 Things You Can See: Notice the wood grain on the desk in front of you. Or the precise shape of your fingernails. Become aware of the glossy green of the plant in the corner. Take your time to really look and acknowledge what you see.
- Become Aware Of 4 Things You Can Touch: The satisfyingly rough texture of the car seat. Your cotton shirt against your neck. If you like, spend a moment literally touching these things. Maybe notice the sensation of gravity itself or the floor beneath you.
- Acknowledge 3 Things You Can Hear: Don’t judge, just hear. The distant traffic. The voices in the next room. As well as the space between sounds.
- Notice 2 Things You Can Smell: If at first you don’t feel like you can smell anything, simply try to sense the subtle fragrance of the air around you, or of your own skin.
- Become Aware Of 1 Thing You Can Taste: The lingering suggestion of coffee on your tongue, maybe?
Repeat this process as many times as necessary. Take your time and notice how you feel afterward. You can also settle down and browse grounding meditations for anxiety relief including guided 54321 practices
There are more therapy procedures that will help you.
Talk to your Metal Health Specialist.

 Tips:
Tips: